

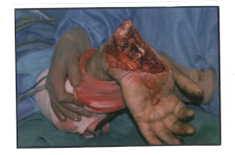
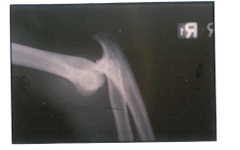
E.G. is a young man who was lending a helping hand in his father’s auto shop when he nearly gave up that hand to a freak accident. He was changing a truck tire when it suddenly exploded causing his elbow to dislocate and nearly amputate his hand. The wrist injury was so severe that it required a surgical fusion once he had been transferred to a Miami Hospital from a more remote location.
The hand surgeon on call had not accepted the transfer due to the severity of the injury, but Dr. Badia was later called and authorized the transfer so that he could perform the reconstruction. E.G.was an inspiration to the other patients in therapy undergoing months of rehabilitation so that he could regain nearly normal motion in his elbow and a functioning hand seen in the comparison photos to his opposite, normal hand

Monday- Friday: 8:30AM- 5:00 PM
Saturday- Sunday: Closed