
Arthrodesis & Arthroplasty
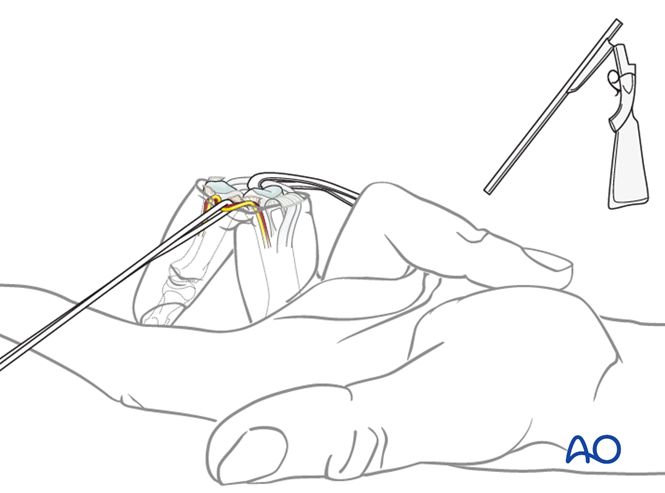
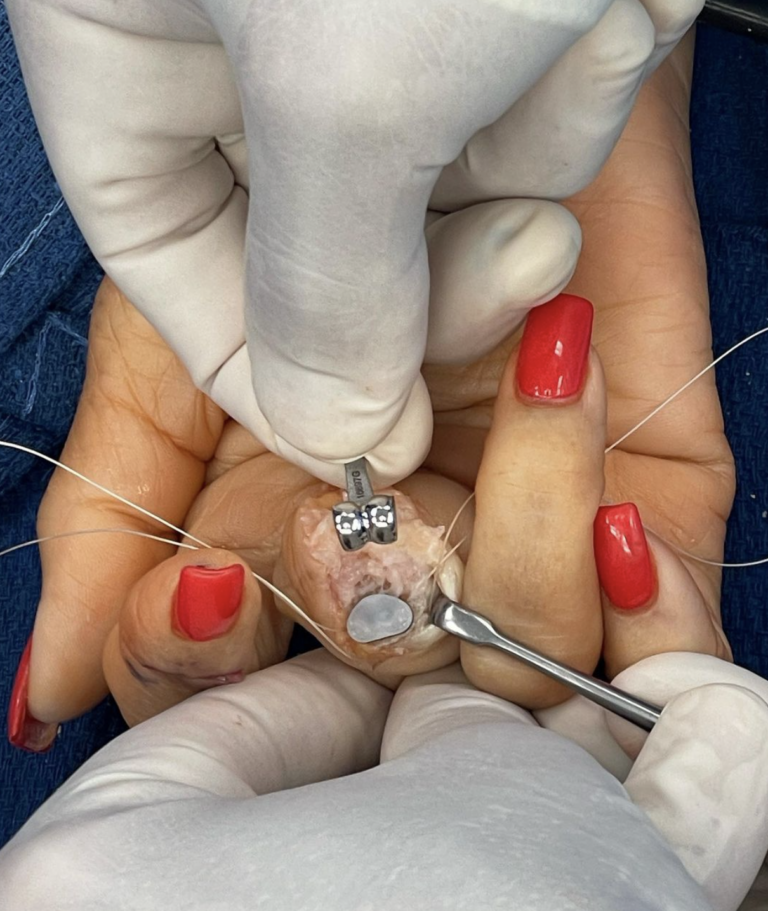
This patient visited our office looking for a solution for arthritis in her fingers. She has experienced exceptional results within a mere 48 hours after undergoing arthodesis (Fusion) and Arthroplasty (Implant) procedures. Her hand is now both functional and esthetic thanks to Dr.Badia’s volar approach (Bruner Incision) .

Monday- Friday: 8:30AM- 5:00 PM
Saturday- Sunday: Closed